Stories of nursing home abuse and neglect aren’t always about a single bad caregiver.
In many cases, there are deeper issues at play, decisions made at the corporate or financial level that shape how care is delivered long before it ever reaches a resident’s bedside.
A decade of in-depth investigative reporting by KFF Health News journalist Jordan Rau, published in partnership with NPR and The New York Times, has uncovered a troubling pattern:
As nursing homes have been absorbed into increasingly complex corporate structures, the money that should go toward patient care is quietly being redirected to investors, landlords, and related companies, leaving residents more vulnerable, and families facing financial devastation.
If you have a loved one in a nursing home, understanding how this works could help you recognize the warning signs of neglect before it’s too late.
The Scale of the Problem
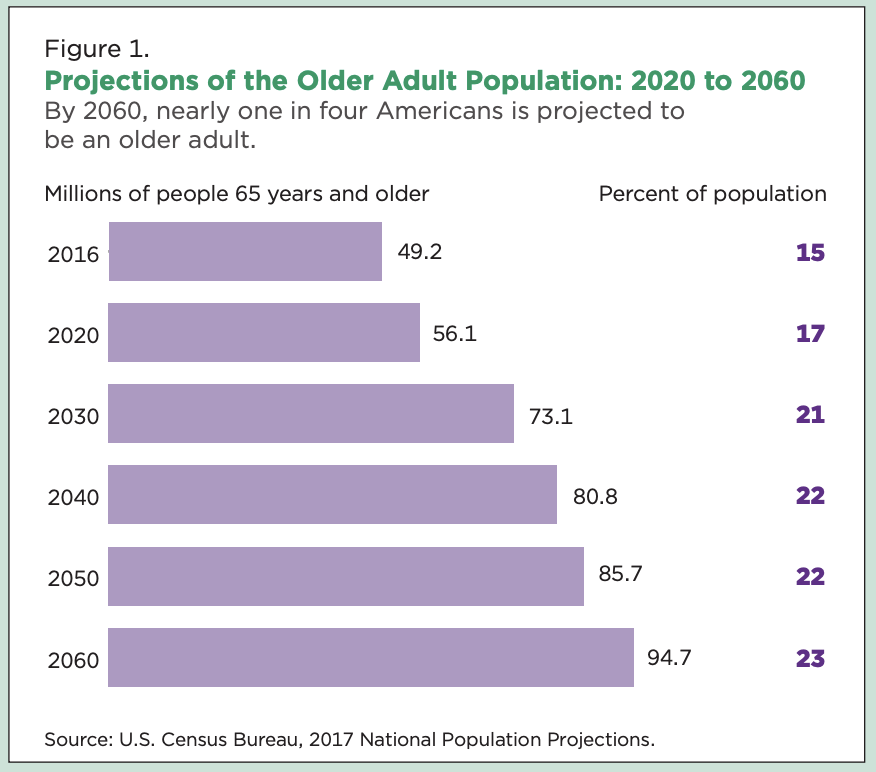
America is aging rapidly, and the demand for elder care is soaring.
By 2030, all baby boomers will be older than 65, causing one in every five Americans to be retirement age. The nation’s 65-and-older population is projected to 95 million people in 2060. The population of Americans 85 and older is projected to nearly triple by 2060, growing from 6.5 million to 19 million people, according to the U.S. Census Bureau’s 2017 National Population Projections.
In 2022 data, more than 1.2 million older adults live in nursing homes across the United States.
Their care is supposed to be the top priority of the facilities housing them. But as investigative reporting has documented, financial interests have increasingly crowded out that responsibility.
What Is a REIT and Why Does It Matter for Your Loved One?
A Real Estate Investment Trust (REIT) is a company that owns income-producing properties and is required by law to distribute most of its profits to shareholders.
Think of it like a corporate landlord, except instead of apartment buildings, some REITs own the physical buildings that nursing homes operate in.
Here’s how it works in practice:
A REIT purchases a nursing home building and then leases it back to an operator, the company that actually runs the facility and hires the staff. The operator must pay rent to the REIT, often at substantial rates.
According to a 2026 NPR/KFF Health News investigation, some REITs extract profit margins as high as 67% from the rents they charge nursing homes.
In 2021, REITs held investments in 1,806 U.S. nursing homes, and when combined with private equity-owned facilities, nearly 30% of all U.S. nursing homes had some form of investor ownership, according to research published in Health Affairs Scholar.
Research has consistently linked REIT ownership to lower staffing levels and worse patient care outcomes.
Corporate Webs: The Bigger Picture
REITs are only part of the story.
They are called related party transactions. Instead of competing in the open market for services like physical therapy, management, drugs, or even building rent, nursing homes pay those costs to companies quietly owned by the same people who own the facility.
As KFF’s reporting put it, “owners can establish highly favorable contracts in which their nursing homes pay more than they might in a competitive market.”
This arrangement allows owners to siphon off profits that never show up on the nursing home’s official books. The nursing home may look like it’s barely breaking even, while the people behind it are quietly earning millions.
When the Money Leaves, Patients Suffer

The financial consequences of these arrangements fall directly on residents.
According to a KFF Health News investigation published by NPR at The Villages of Orleans in western New York, private investors collected nearly $16 million in rent from their own nursing home over seven years, paid to a real estate company they also owned, while residents fell without help, developed bedsores, missed medications, and were left in soiled diapers for hours. Part of a ceiling collapsed on a nurse. The state attorney general eventually sued.
At Fulton Commons Care Center on Long Island, the owner later admitted under oath that he had never once set foot inside his nursing home. His family still collected nearly $16 million over four years through inflated rent, management fees, and jobs created for his eight children.
Meanwhile, residents’ family members reported loved ones left sitting without proper clothing, suffering untreated infections, and waiting over an hour for staff to respond to a call bell.
The Financial Exploitation Families Face
The financial pressure of REIT and corporate ownership does not just affect resident safety, it directly impacts families who are already stretched thin.
Long-term care costs in America are staggering. According to the 2025 CareScout Cost of Care Survey, here is what families are actually paying:
- A semi-private nursing home room costs a median of $9,581 per month, more than $114,000 per year
- A private nursing home room runs $10,798 per month, or over $129,000 annually
- Assisted living communities average $6,200 per month, $74,400 per year
- Memory care units average $8,019 per month, or roughly $96,000 per year
- A non-medical home caregiver costs a median of $35 per hour, totaling over $80,000 per year for full-time care
For most families, these costs are simply not sustainable, especially when the facility draining their savings is simultaneously funneling money to related companies owned by the same investors.
On top of these already-crushing costs, financially motivated facilities sometimes add to families’ burdens through:
- Improper billing and upcoding, charging for services that were never provided
- Hidden fee structures, routine services that families assumed were included often come with additional charges not disclosed upfront
- Complex corporate structures that make it extremely difficult to hold owners accountable in court, because money has already been distributed to related entities by the time a lawsuit is filed
Even Staffing Laws Aren’t Enough
Many families assume that minimum staffing laws protect their loved ones.
But a KFF Health News investigation found that nursing homes routinely fail to meet even the toughest state standards, with little consequence.
As one long-term care ombudsman told KFF Health News: “Just setting a number doesn’t mean anything if you’re not going to enforce it.”
States regularly grant waivers and exemptions, enforcement depends on underfunded health inspectors, and penalties for violations are rarely imposed.
When ownership structures are designed to pull money out of a facility, there is simply less left over for staffing, and no law on the books changes that math.
Residents are left to absorb the consequences, even in facilities that appear compliant on paper.
Warning Signs to Watch for in Arizona Nursing Homes
If your loved one is in a nursing home, here are warning signs that financial pressures may be compromising their care:
- Frequent staff turnover — New faces every visit often signal low wages and poor working conditions
- Understaffing — Call lights going unanswered, long waits for basic assistance
- Unexplained weight loss or dehydration — Signs residents aren’t getting adequate help with eating and drinking
- Bedsores or skin breakdown — One of the clearest markers of neglect, and a sign of inadequate repositioning
- Inaccurate records — Notes that don’t match what families observe during visits
- Billing discrepancies — Charges for services your loved one didn’t receive, or pressure to pay amounts Medicare/Medicaid should cover
How Miller Kory Rowe LLP Can Help
When a nursing home’s financial structure leads to neglect, whether through understaffing, misallocated resources, or deliberate indifference, the residents who suffer and their families have legal rights.
At Miller Kory Rowe LLP, we investigate the full picture. That includes looking beyond the facility operator to understand whether the ownership structure contributed to the dangerous conditions your loved one experienced. Holding nursing homes accountable doesn’t just compensate victims and their families, it forces systemic changes that protect future residents.
If you believe your loved one has suffered neglect or abuse in an Arizona nursing home, contact Miller Kory Rowe LLP today at (602) 560-9595 for a free consultation.
Sources
1. Rau, J. (2026, April 21). Real estate investors profit from long-term care while residents languish. KFF Health News / NPR. https://kffhealthnews.org/health-industry/real-estate-investment-trusts-senior-housing-nursing-homes-profit/
2. Rau, J. (2017, December 31). Care suffers as more nursing homes feed money into corporate webs. KFF Health News / The New York Times. https://kffhealthnews.org/news/care-suffers-as-more-nursing-homes-feed-money-into-corporate-webs/
3. Rau, J. (2023, January 31). Nursing home owners drained cash from understaffed facilities. NPR. https://www.npr.org/sections/health-shots/2023/01/31/1139783599/new-york-nursing-home-owners-drained-cash
4. Abelson, R., & Rau, J. (2023, November 14). Facing financial ruin as costs soar for elder care. KFF Health News / The New York Times. https://kffhealthnews.org/news/article/dying-broke-facing-financial-ruin-as-costs-soar-for-elder-care/
5. Brayn, R. T., et al. (2024). Nursing home finances associated with real estate investment trust and private equity investments. Health Affairs Scholar, 2(4). https://academic.oup.com/healthaffairsscholar/article/2/4/qxae037/7645605
6. Braun, R. T., et al. (2022). The role of real estate investment trusts in staffing US nursing homes. Health Affairs, 41(7). https://www.healthaffairs.org/doi/10.1377/hlthaff.2022.00278
7. Rau, J. (2023, November 20). Extra fees drive assisted living profits. KFF Health News / The New York Times. https://kffhealthnews.org/news/article/dying-broke-extra-fees-drive-assisted-living-profits/
8. Rau, J. (2024, July 12). States set minimum staffing levels for nursing homes. Residents suffer when rules are ignored or waived. KFF Health News / The New York Times. https://kffhealthnews.org/news/article/nursing-home-minimum-staffing-state-laws-enforcement-residents-suffer/
9. Elwell, F. (1982). Profits and patient care quality in nursing homes: are they compatible? Journal of the American Geriatrics Society, 30(7), 448–450. https://pubmed.ncbi.nlm.nih.gov/6802706/
